
“How does the pain feel?” When patients are asked this question by their doctor, they want to answer as accurately and precisely as possible. Unfortunately, they often lack the right words to describe the pain in the back, head, or under the skin. “This is the case for every second one of my patients,” confirms Dr. Karl Wohak, head of the interdisciplinary, multimodal pain center at the Private Clinic Wehrle-Diakonissen in Salzburg. Every day, he sees people suffering from chronic pain, meaning their pain has tormented them for more than six months despite therapy. “Unlike obvious and acute sources of pain such as inflammation or injuries, chronic pain usually involves nerve damage, a dysfunction of the nerves. Diseases like diabetes, Morbus Sudeck, spinal wear and tear, or the aftermath of shingles can cause this nerve damage. Likewise, internal scarring post-surgery can irritate and overstimulate nerves and nerve roots, leading to persistent pain. Because these causes are not visible, it helps the doctor if the patient can describe their pain as precisely as possible. The nature of the pain can indicate its source.”
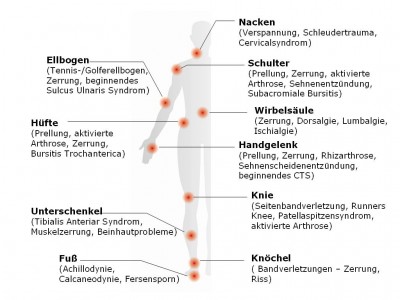
However, many patients struggle to find the right words. Pain therapist Dr. Reinald Brezovsky often encounters this. “Many people simply aren’t eloquent. Others have never thought about describing the nature, intensity, and location of their pain. Some are so nervous during a doctor’s visit that they’re at a loss for words.”
Good communication between doctor and pain patient not only leads to faster diagnosis but also prevents unnecessary therapies and facilitates swift referral to the right specialist. “If a patient says they feel like their ankles are in a vise and they experience tingling or burning in the lower legs, it’s likely polyneuropathy. This is nerve damage that can be caused by diabetes or chemotherapy, for instance. The patient can immediately be referred to a neurologist, who will conduct further examinations and suggest appropriate therapies,” explains Dr. Brezovsky. Therefore, it makes sense to think about the pain at home and in peace. “This includes when the pain started, how long it lasts, where it is felt, and what sensation it causes. Writing this down and bringing the notes to the doctor’s visit supports general practitioners, specialists, and even specialized pain doctors in their work. I also recommend always noting down which medications have been taken for pain treatment,” advises Dr. Wohak.
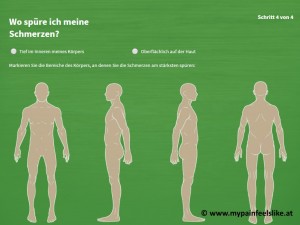
For those who still can’t find the right words despite all efforts, the internet offers questionnaires with examples of how pain can feel. On the website www.mypainfeelslike.at, such a questionnaire is available for printing. It features about two dozen visually described types of pain. If a description matches one’s own pain, it just needs to be checked. Multiple mentions are possible. It spans four pages and even includes a graphic where sufferers can mark the spot that causes them pain. Those without internet access should ask a family member or a friend to print a questionnaire for them. “Many chronic pains can be better managed the sooner their cause is identified and the right therapy is started. This prevents late effects such as depression and the social isolation of the pain patient,” says Dr. Brezovsky.

